What is COVID-19 Coronavirus?
The COVID-19 Coronavirus is a new type of coronavirus that has been transmitted from bats in a local market in southern China. With symptoms that vary from a common cold to a more Severe Acute Respiratory Syndrome (SARS), the COVID-19 has continuously been compared to the SARS outbreak nearly two decades ago. Nevertheless, the similarities between the two cases are mostly in the fact that both illnesses are caused by air transmitted viruses. However, they differ immensely in how they act in the human body and the level of severity of contamination. For the present COVID-19, the virus has been identified, and detection tests have been developed being non-invasive and precisely identifying individuals that are contaminated or not. Unfortunately, there is no vaccine or specific medicines developed for the virus infection up to this point.
As COVID-19 mostly acts on the body as a common cold, it is recommended that individuals presenting any symptoms be redirected to hospitals for screening, quarantined, and only after clearance be allowed to interact with large groups again. Although the virus most frequently does not evolve to fatal cases, elders, children, or individuals who already possess other respiratory issues, are considered to be patients at-risk and should be monitored closely in a controlled environment. The disease can evolve rapidly, creating difficulties in breathing, and over 800 individuals have deceased from infection-related complications.
See Big Red in Action: Bio Decontamination During SARS in Singapore
What’s the Difference Between the COVID-19 Coronavirus and SARS?
The global outbreak of SARS in 2003 affected over 8000 people in 37 different countries and set the grounds for the worldwide epidemic of this new millennium. With the advent of globalization, increase in air traffic and other transportation modes, a simple viral infection can find ways of spreading globally much faster than science and medicine can keep up with its treatment and prevention. The lessons from the 2003 SARS incident are now continually being recalled as governments and policies struggle to control and contain the transmission of the COVID-19.
Debates on the previous SARS outbreak are also common due to the similarities between the two viruses, which can help provide better solutions to the several proposals for containment and control. Genetically, SARS and the COVID-19 are 70% similar, both causing flu-like symptoms. When infected, individuals soon develop fever, malaise, dry cough, headache, chills, and muscle aches. For those who already have conditions that present weak immunity, both infections have been known to cause pneumonia.
Another similarity is that both viruses are zoonotic, which means they were transmitted from animals to humans. Both the viruses were also pointed out to be transmitted specifically by bats in local markets and areas where the cuisine practice the consumption of these animals. Once infected, humans work as carries for the infection and tend to spread it through the air by coughing and sneezing.
Transmission between humans, therefore, happens considering a direct transfer of the virus from one body to the next, needing no intermediary species for this transmission to occur. In other words, individuals that are infected are able to transmit the virus through saliva when they cough and when they sneeze. The droplets released can either be inhaled by individuals who are closed to them, or can deposit in surfaces and tabletops in their surroundings. These droplets are then transferred through a direct transfer, where non-infected individuals touch these surfaces and bring the virus through their bodies by touching their mouths, eyes, and mucosa.
What are the Forms of COVID-19 Coronavirus Contamination?
Contamination of the COVID-19 virus occurs by inhaling or contacting the virus that is transported in the air through droplets from the contaminated individual to new individuals and surfaces. When an individual is contaminated, all its saliva and internal respiratory system are filled with the virus. As he coughs as sneezes, the virus leaves the host body and enters the air. If not immediately inhaled by other individuals, it will deposit on surfaces and wait for someone to touch it and inhale it through direct transmission.
In other words, when contaminated individuals cough or sneeze in a specific area, all their surroundings are prone to be infected with the virus that slowly deposits on the surface. These tabletops, buttons, hand knobs, and others can serve as a pool waiting for new individuals to touch them and transfer the virus to the body by inhaling it themselves. This means that even if you are not in direct contact with a contaminated individual, you might be exposed to the virus if he or she has been in the same room you are in.
Moreover, as most flu-like symptoms lead to sneezing and coughing, which cause a reflect reaction of “bringing your hands to your mouth,” the hands are specifically high contamination points. As we cough and cover our mouths with our hands, we also transfer large amounts of the virus to our hands. By consequence, materials and objects that are continuously handled by a large number of individuals are the highest risks in any environment. In other words, elevator buttons, doorknobs, handles, and stair supports are all extremely contagious objects that should be avoided.
Unconventional routes of contamination should also be considered as previous cases with SARS showed that several unexpected infections occurred through means that were previously ignored. For example, contamination through sewage vents has been reported associated with droplets forming from moist conditions in these environments that allowed for the disease to be carried along in the form of droplets.
How Long Does the COVID-19 Coronavirus Last on a Surface?
Typically, the coronaviruses can live on the surface, waiting to infect a new host for nearly three days. If left untouched, this means that the coronavirus lays dormant on surfaces for over two years until the next host comes in touch with it and restarts the infestation process. That is why it is imperative to carry out adequate disinfection of surfaces in all areas where contamination might be at risk.
One of the common mistakes noted with surface disinfection is the use of inadequate materials and chemicals to carry out this process. Most people believe that alcohol is an efficient disinfectant, and that is capable of cleaning out the surface of the risk of coronavirus infection. However, this is not the case.
Alcohol and other over-the-counter disinfectant are capable of eliminating most microbes and microorganisms that create smell and stain in local homes and office buildings. These are used in order to avoid the proliferation of microbial colonies that might cause several allergic reactions and eventually, sick building syndrome (SBS), which affects innumerous establishment worldwide.
However, due to the biological properties of the COVID-19 Coronavirus, most of these products are ineffective towards the virus and unable to kill it. On the other hand, they kill all the other living organisms found on the surface, leaving it no competition. Hence, inadequately cleaning of these surfaces might even promote a longer life for these viruses allowing them to increase their retention time on the surface top.
Additionally, manually do it yourself (DIY) cleaning processes rely intensely on the use of wipes, which serve to spread the chemicals on the surface and remove the accumulated dust. Although quite efficient for dust removal and to improve aesthetical value for the office space and household, this process is highly dangerous and increases the risk of COVID-19 infection. Here, as the individuals apply the wipes on the surface and spread the chemicals throughout the area, they also induce mechanical transfer of the virus from that surface to other areas. As untrained cleaners continue the process through different rooms, the virus is carried out through the building, increasing their chances of infection.
Learn more: Coronavirus Outbreak – What to Do?
How Long Do Particulates and Aerosol Carrying COVID-19 Coronavirus Stay in the Air?
Estimating the time that a particulate or aerosol with coronavirus can be found in the air is a very complex task. These values vary according to temperature, humidity, wind, and also the volume of viruses that got released in the air at once. In any case, it is essential to keep in mind that the coronavirus can survive outside the human body for nearly three days, being capable of contaminating a second individual within the first moment they come into contact. Therefore, it is vital to keep all areas well ventilated to avoid touching surfaces of high risk and to carry out quarantine measures in case individuals are found contaminated within your surroundings.
In other words, if your home building, school, office or commercial building has seen the incidence of coronavirus among any of their occupants, it is essential to evacuate the area and carry out professional disinfection of the surfaces, air ducts, air vents and filters throughout the building that might help transport, accumulate and transmit the virus to other individuals and infrastructures.
How to Eliminate the COVID-19 Coronavirus from the Surface?
For areas that have confirmed cases of infections or transmissions or in the regions that are typical of high risk due to intense circulation, professional disinfection is recommended. When reaching out to professional disinfection teams, the managers and responsible for these areas are required to carry out shutdown and evacuation of the area to avoid any cross-contamination. The off period will last as long as the disinfection team requires due to the risk of contamination from the specialized chemicals used.
As for the disinfection team, a set of personal protection equipment (PPE) is required which extend from shoe covers to facial mask and eye protectors allowing these individuals to enter the environment without any personal risk of infection. The trained personnel is then responsible for carrying thorough disinfection of the area using proper equipment and chemicals which require specific training for handling.
Note here that besides protecting themselves, these trained individuals are also responsible for preventing cross-contamination between rooms to occur, paying special attention to the cleaning process as to not allow for extensive use of wipes and other materials that might transfer the virus. Once the procedure is finished, a clearing period is required so that the level of chemicals in the air is reduced to safe levels, and regular operation can be restored.
As a precaution measure, processes of Antimicrobial Surface Coating can also be applied, seeking to avoid the sedimentation of these viruses. These coatings can be found in powder, liquids, or pellets and represent an effective way to inhibit the proliferation of microbial on any surface or countertop. Through the addition of silver ions, zinc, or copper, antimicrobials can be built-into almost any surface, and due to their chemical properties, help to keep the surface clean and free from any microbial organism.
What Temperatures Favor the Reproduction of COVID-19 Coronavirus?
Although several doctors associate the coronaviruses to a more winter-time disease, there is no scientific proof that determines a tendency to higher reproduction during winter or summer times. As several tropical countries like Singapore have already started reporting the incidence of COVID-19, it is safe to say that there is no valid correlation between temperature and reproduction rates of these viruses.
How Does Coronavirus Act in your Body?
Coronavirus causes flu-like symptoms that grow as the days pass by. Initially, the feeling of a dry, sore throat occurs, which can last for up to 4 days. By then, the virus transfers to your nasal fluids and trachea, reaching the lungs, which can lead to a case of pneumonia, a process that lasts around five days. Pneumonia is usually linked to high fever, problems in breading, nasal congestion, and others, which will most likely require medical attention.
Most cases of death after the pneumonia is installed due to improper treatment of the disease or individuals that already presented a deficient immune system or respiratory system due to other illnesses. In this case, most individuals who have been reported to dye from the COVID-19 are elders and young children who were at higher risk of developing complications in their respiratory system.
When Should You Use a Mask?
Although the mask helps to prevent the transmission from contaminated individuals to others, the virus can not be considered airborne, and therefore does not survive in the air like a suspended particle. Due to its large size, the COVID-19 is most likely released from the host immersed in droplets that are coughed out of the infected host. These droplets remain very briefly in the air finding themselves deposited on surfaces directly in the path of the cough.
Nevertheless, when these droplets hit random surfaces, they tend to fixate and remain as a contamination risk for nearly three days on that surface. In this sense, the highest risk of contamination is not found in an airborne situation, but in surfaces that are frequently touched by contaminated individuals. Hence, elevator buttons, doorknobs, bathroom locks, and others are much more likely to represent significant contamination risk than the air surrounding the infected itself.
Moreover, as humans present an automated reaction of covering their mouths as they sneeze or cough, they commonly carry the virus in that contact and deposit it on the next surface they touch. In most places with a high circulation of crowds, these are the areas intended for manual contacts like handles, supports, doorknobs, and others.
What to Do in Code Red Scenarios?
As more unlinked cases are identified from contaminations occurring in the Singapore area, the government has officially increased the alert to code orange. The same code was used in the H1N1 outbreak and cause several different inconveniences for the population.
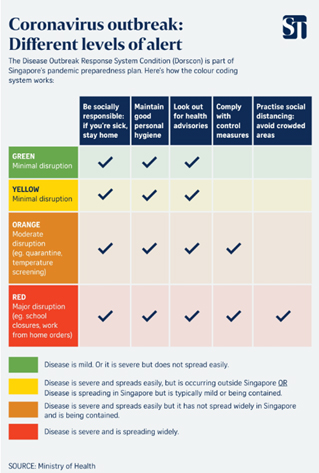
At code orange, the population is being required to avoid crowded events and spaces of intense circulation. The government is also requesting daily health checks at workplaces and several additional measures that seek to protect vulnerable groups such as children at schools and pre-schools and individuals in healthcare institutions.
In case the alert does escalate to code red, local commerce, business offices, and services will suffer great restraint as the government urges people to avoid contact in highly densely populated areas.
Is the COVID-19 Coronavirus Outbreak a Pandemic?
The World Health Organization has not yet stated that the coronavirus outspread is to be considered a global health emergency. Still, a significant consideration is being carried out on the issue as the numbers continue to climb. According to the WHO, pandemics are considered to happen when influenza viruses emerge and spread throughout the entire globe, which is most likely the case of the COVID-19 if the situation continues to escalate at this rate. On the other hand, a national pandemic in China is already considered to be occurring.
